
Clinical Prognostication and Diagnostics of Neurological Disorders

We analyze how neuroscience technology, including: the KINARM exoskeleton, MRI, functional MRI, EEG, and markerless motion picture gait analysis, can be used for prognostication and as adjunct diagnostic tools. Specifically, the similar presentations of normal pressure hydrocephalus, cervical myelopathy, and Parkinson’s disease providing a unique diagnostic challenge has become a focus of our labs work. Our findings aim to influence clinical practice and streamline neurosurgical care.
Integrating Biopsychosocial Insights into Neurosurgical Outcomes
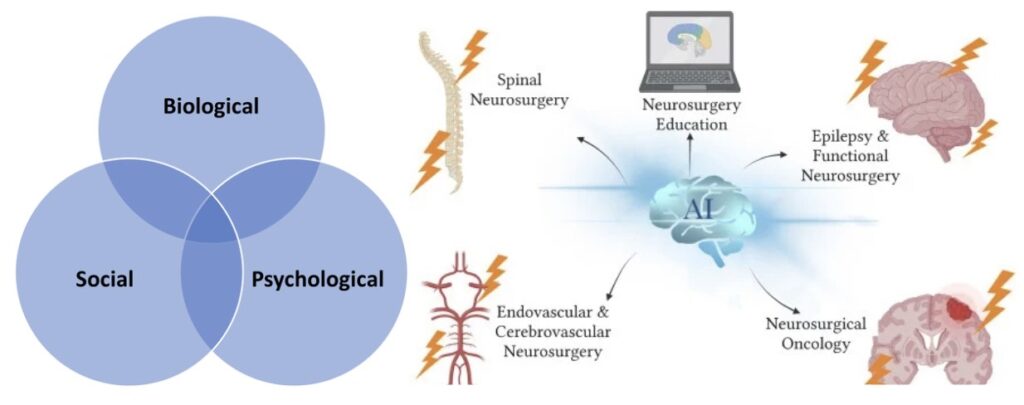
We investigate how biological injury, psychological recovery, and social context jointly shape postoperative trajectories. Leveraging population-level health databases and mixed-methods cohort studies, the team maps geographic, socioeconomic, and Indigenous disparities that influence access to neurosurgery and long-term functional recovery. These findings inform equity-driven policy and patient-centred innovations.
Language-Based Biomarkers of Neurodegeneration
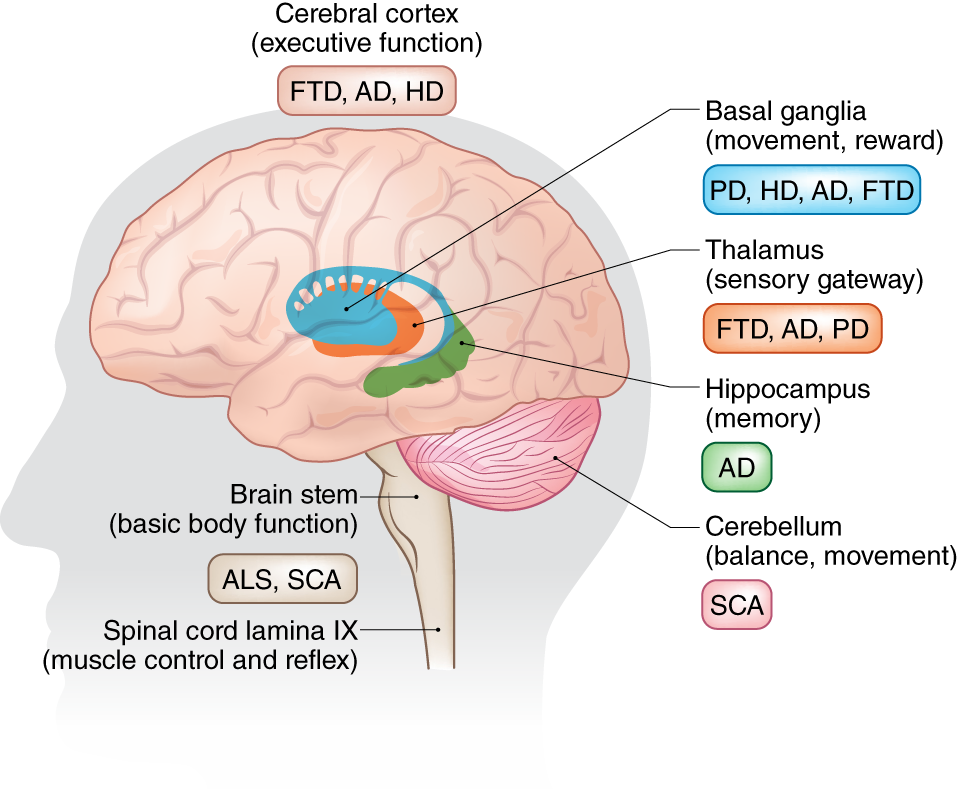
Using large-language-model natural-language-processing pipelines, we quantify subtle shifts in lexical diversity, emotional valence, and syntactic complexity that emerge with cognitive decline. By coupling longitudinal speech samples with clinical metrics, our work aims to build non-invasive, scalable tools for early detection and monitoring of neurodegenerative disorders.
Optimal Surgical Pathways and Systems Performance
Through health-services analytics, we identify bottlenecks in pre-operative referral networks and day-of-surgery workflows at regional trauma centres. Predictive modelling and stakeholder-informed intervention design guide strategies that reduce cancellation rates, streamline care pathways, and enhance operating-room efficiency, ultimately improving surgical access and outcomes across the continuum of care.